
Most cost containment solutions start after the fact. A member gets care, a claim is filed — and only then does someone try to reduce costs.
To fix this, Goodbill built ClearAccess in partnership with two industry leaders, ClearHealth Strategies, a pricing solution, and BillingNav, which specializes in resolving unexpected bills — blending the best of our capabilities into a solution that guides members to affordable, high-quality care, helps prevent unexpected charges, and drives savings across the healthcare journey.
This week, Nationwide announced the rollout of ClearAccess to help their self-funded plans contain costs from the moment a member searches for care. This marks our first deployment of this solution with a Fortune 100 carrier — and a major step forward in how Goodbill helps plans manage costs across the full member journey.
“This solution provides our customers with cutting-edge member navigation to help them effectively search for care options and eliminate unexpected costs,” Casey Lanto, head of Nationwide Group Benefits Product and Operations, said in the announcement.
“Navigating a health plan and the healthcare system can be confusing. Packaging the ClearAccess tool with Nationwide’s Self-Funded Program means members are getting a clearer, more affordable care experience.”
With this rollout, we’re driving savings across the full journey for self-funded groups:
“Employers are told to choose between lower costs and a good member experience. We don’t think that’s true,” said Patrick Haig, co-founder and CEO of Goodbill. “When you help members find high-quality but affordable care, costs come down for everyone.”
Plans often overspend because members make uninformed decisions. Members choose providers without knowing the cost. They miss benefits included in their plan. Discounts go unused.
ClearAccess changes that by getting involved earlier, and staying involved throughout. Here’s what that looks like in practice:
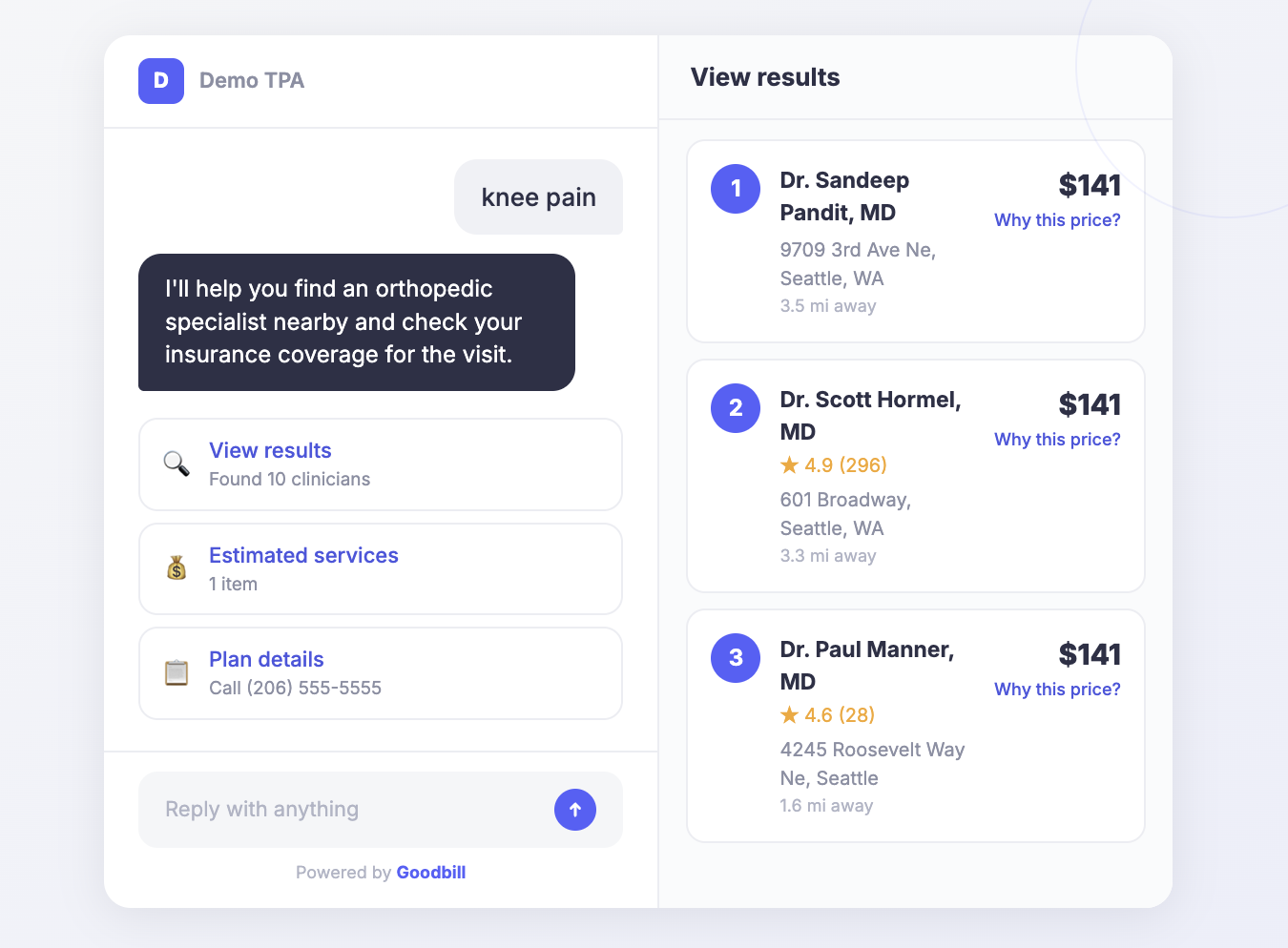
When a member searches for care, we evaluate each provider’s rates and billing history to surface the best option and enable direct booking in just a few clicks.
We understand the details of each member’s plan, so we can guide them toward covered services, preventive care, and lower-cost care pathways they might otherwise miss.
We screen every hospital claim for discounts and savings opportunities before the claim is paid.
If a member receives an unexpected bill, we work to resolve it, while ensuring the member continues to receive access to care.
If you’re a broker, TPA, or employer interested in how our ClearAccess solution can help your self-funded plans, book a demo at goodbill.com/demo or email partner@goodbill.com.
Guides, news, and articles to help you tackle hospital bills.

Plan fiduciaries don’t need to look very far. Substantial savings are likely hiding in their claims today.

Goodbill CEO Patrick Haig joins the Business of Benefits podcast.

Goodbill’s solution helps Optimyl clients reduce hospital charges before they pay providers.